In this article, we’ll cover the current realities of the revenue cycle management process in medical billing (RCM) from beginning to end. We’ll outline some key issues affecting medical billing workflows along with steps you can take to improve your company’s IT systems and financial performance.
Let’s face it: medical billing is fraught with problems. Decision makers and billing managers face a myriad of challenges, from transitioning from manual processes and maintaining compliance with various rules and regulations to reducing errors and costs. However, some of the biggest issues are the easiest to address.

What is RCM in Medical Billing?
Revenue cycle management in medical billing (RCM) is a process through which clinical management systems interact with medical billing systems. These billing systems exchange information between clearinghouses, patient statement systems and patient payment vendors to complete a financial transaction between healthcare patients, providers and payers.
Current Revenue Cycle Management Workflow
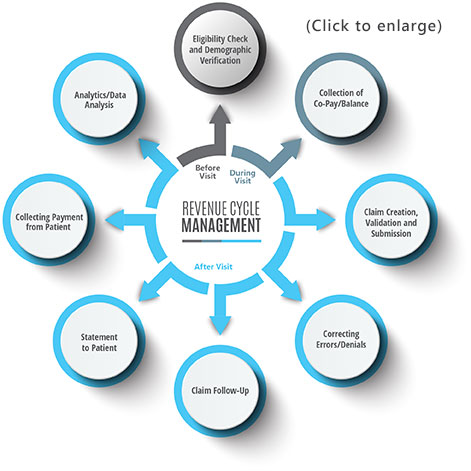
The RCM workflow from beginning to end consists of the following eight medical billing cycle steps:
Step 1: Eligibility Check and Demographic Verification: Ensuring patients have valid insurance coverage prior to scheduling an appointment
Step 2: Collection of Co-pay/Balance: Collecting a fixed amount from a patient at time of service as well as the amount owed from a prior visit that wasn’t covered by a patient’s insurance
Step 3: Claim Creation, Validation and Submission: Manually or electronically creating claims and submitting them to the insurance provider, a clearinghouse or another type of claims vendor
Step 4: Correcting Errors/Denials: Determining if a claim needs to be corrected and resubmitted or if additional documentation is required. Some insurance providers also have a specific appeal process, deadlines or a timely filing limit you must meet to be successfully reconsidered.
Step 5: Claim Follow-up: Reaching out again to the payer via phone, email, letter or online. When done correctly, following up can substantially reduce days in A/R and ease unnecessary financial burden on patients.
Step 6: Statement to Patient: Sending the final costs to a patient as a printed or electronic bill, including demographic details, the amount owed, date of the procedure and transaction descriptions
Step 7: Collecting Payment from Patient: Mobile and online payment are two methods used today to simplify patient collections. It’s important to consider the needs of your staff to fulfill basic requirements, such as automatic posting and reconciliation.
Step 8: Analytics/Data Analysis: Processing and aggregating data into meaningful insights to improve business operations in the form of increased collections, reduced days in A/R and stable financial performance
Are you still relying on a manual billing workflow? Learn how new technologies are being used for greater efficiency in our ebook, "How Automation Could Improve Your Revenue Cycle."
Key Issues and Corresponding Steps for Improving Medical Billing in RCM
Understanding the key issues in improving medical billing in RCM is the first step in improving the process. By identifying these issues and implementing a solution to fix them, you’ll experience improved revenue, quicker reimbursement and other advantages.
Issue #1: Siloed Steps in Your Revenue Cycle Process - Almost 70 percent of healthcare organizations use multiple vendors for their RCM processes, and 30 percent of hospitals and health systems are unable to successfully handle their revenue cycle automation efforts without at least two vendors. In the confusion of managing multiple vendors, though, some organizations overlook duplicate features available in their current software.
- How to Improve: Spend some time auditing your current RCM services. Look for opportunities to integrate systems, which enables your clinical experience to communicate with your billing management software, which in turn communicates with your clearinghouse, patient payment system and statement vendor. Connecting your patient electronic health records (EHRs), billing information, clearinghouse, patient payment portal and statement vendor can help you reclaim lost revenue.
Issue #2: Backed Up Medical Billing Workflow During Admission, and After a Patient’s Visit - Time-consuming paperwork and manual processes are two of the largest contributors to inefficient claims management.
- How to Improve: Switch from paper to electronic statements (e-statements) while still giving patients who prefer paper statements the option to receive one. Just make sure that you’re only sending the number of paper statements necessary to receive payment from patients who are most likely to pay.
Issue #3: Denied and Rejected Claims Management - Average claim denial rates range from 6-13 percent, and 65 percent are never resubmitted. An estimated 90 percent of denials are preventable. Common causes of claim denials include missing or incorrect data, duplicate or late submissions, improper or outdated CPT or ICD-10 codes and lack of documentation or prior authorization.
- How to Improve: Employ a three-pronged approach. First, optimize processes for insurance verification and eligibility. Second, train your staff on crucial conversations regarding patient payment obligations and payment options. Third, transition to better IT software to reduce unnecessary delays between claim filing and patient billing.
Issue #4: Adapting to Changes in ICD Codes - There are five times the number of medical diagnosis codes in ICD-10 - roughly 69,000- as there were in ICD-9. Traditionally adapting to changes in ICD codes relied almost entirely on continual training, resulting in staff turnaround and additional overhead. Challenges will increase with value-based requirements for more robust clinical documentation.
- How to Improve: Utilize automated coding and machine learning software, which can learn from past diagnoses codes compared to their rate of successful claim submissions. Auto-populate new claims with the same information, thereby ensuring a higher success rate in a fraction of the time.
Issue #5: Revenue Data Loss, and a Lack of Healthcare Analytics - Measuring outcomes is interesting, but not always actionable for improving productivity in your revenue cycle process.
- How to Improve: Use business intelligence in the form of roll-up reporting, real-time data processing and intelligible dashboards. It’s great to know your percentage of clean claims, but it’s even better to know your top sources of denied claims. One metric shows you how well your company has performed in the past. The other metric displays how your company could perform better in the future.
The Benefits of Selecting ImagineSoftware
We offer the first intelligent, multi-specialty medical billing software. Our ImagineBilling™ solution simplifies billing processes, automates charge and claim management, monitors productivity and more. Plus, our claims management solutions enable healthcare organizations to quickly create, send and track claims within an approval system configured to employees’ preferred workflows. Contact us to learn more!