Get Automated
Quickly create, send and track claims within an approval system configured to employees’ preferred workflows. Automate processes for high volume, low touch claims and receive transactional data overnight for morning review. Flag unusual claims and prevent future issues with machine learning.
What's stopping you from upgrading your claims management solutions?
-
“Our legacy system has its bugs but works fine.”
“Works fine” isn’t good enough. Debug your legacy system with a multi-specialty interface engine at $0 cost.
-
“Our system architecture is so complex. Changing would disrupt the business.”
Change systems with minimal disruption and no data loss. We’ll run your current and new systems in parallel to make conversion seamless and easy.
-
“Our previous implementation was a disaster. I’m not sure we’re ready to get into one again.”
With 20+ years of experience connecting with third-party EHR, RIS, LIS, HIS, and clearinghouses, we make implementation painless.
-
“We don’t want to be locked into using features and software we don’t need.”
Keep your current vendors or choose from a list of our preferred partners – you get complete flexibility.
Get your claims out quicker to keep payments coming in
| INDUSTRY METRICS | INDUSTRY AVERAGE | |
|---|---|---|
| Days in A/R | 49 | 35 |
| Net Collections | 85% | 97% |
| A/R > 120 | 25% | < 15% |
| Denials | 9.7% | 6.5% |
| Productivity | 28K | 40K |
| Coding Audit | 88% | 95% |
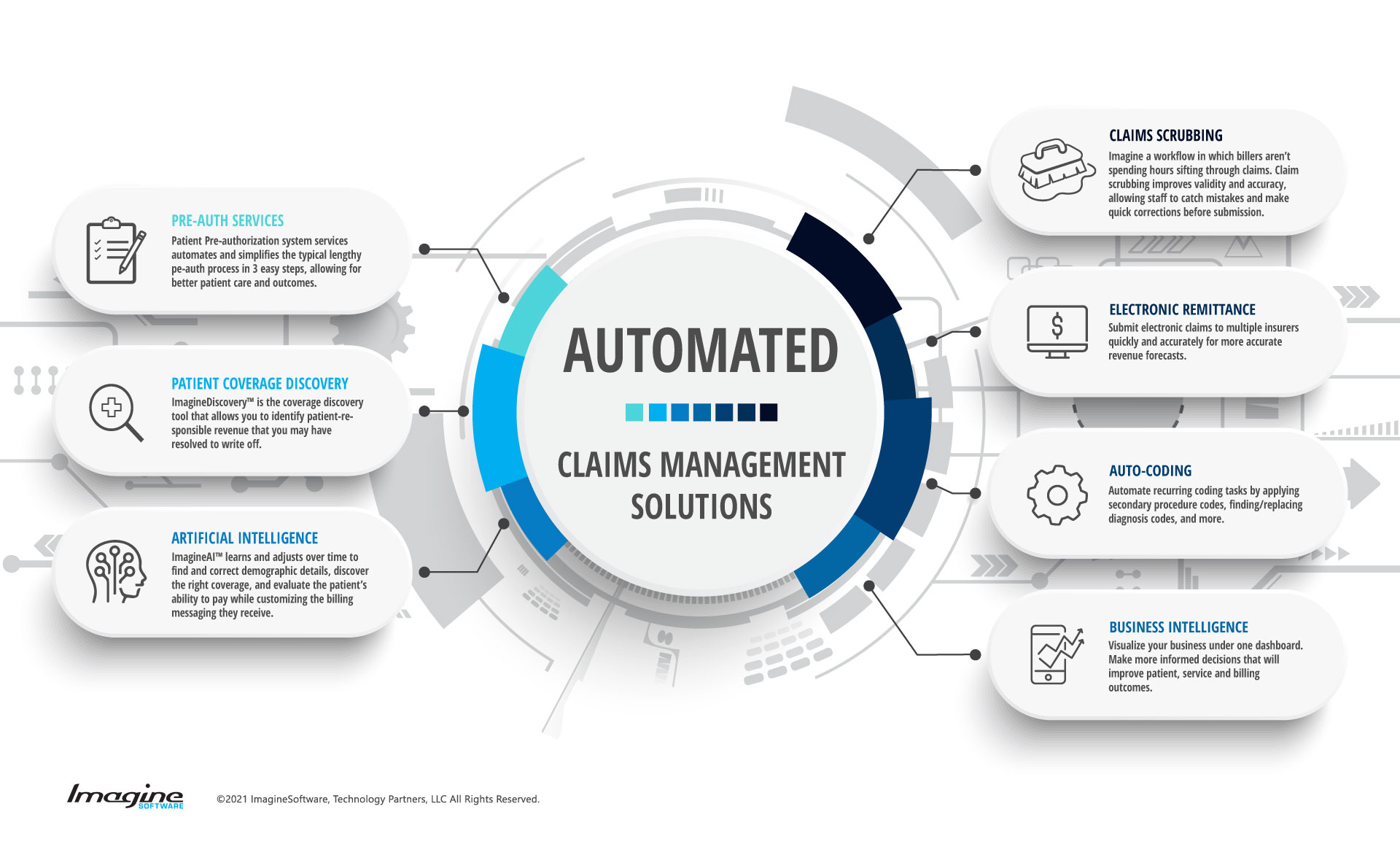
Get Efficient With:
Automatic Worklists
On-the-fly Editing
Claims Scrubbing
Artificial Intelligence
Business Intelligence
"Everything used to be manual. Using ImagineSoftware we’ve been able to send out claims and get payment electronically from the bulk of our payers. We have gained a lot of efficiency through automation."